Cataract Surgeon
Adjunct Professor Hemal Mehta
Dr Mehta is a highly experienced cataract surgeon having performed thousands of operations.
He has written National guidelines on the management of cataract in patients with macular disease. Dr Mehta tailors cataract surgery according to the individual’s needs to help them achieve the optimal outcome. He ensures patients are supported throughout their journey from pre-operative assessment, to cataract surgery and then post-operative recovery.
Intraocular lens choices
During cataract surgery, the cloudy lens is replaced with a new clear intraocular lens in the eye. There are a range of lens options available according to the patient’s requirements. Dr Mehta will discuss the most suitable lens choice with you before cataract surgery.
Monofocal intraocular lenses offer the highest quality vision but are limited to a particular focal length. Therefore, patients set for clearer unaided distance vision would require glasses for reading and computer tasks.
Monovision describes the situation where one eye is set for distance vision and the other for reading vision. There is only so much difference in focal length between the eyes that the brain will tolerate. Therefore, monovision is preferred in patients who already have a prescription where one eye sees more clearly in the distance and the other eye sees more clearly for reading tasks. Otherwise, it is recommended to have a contact lens trial simulating monovision before committing to this arrangement in cataract surgery.
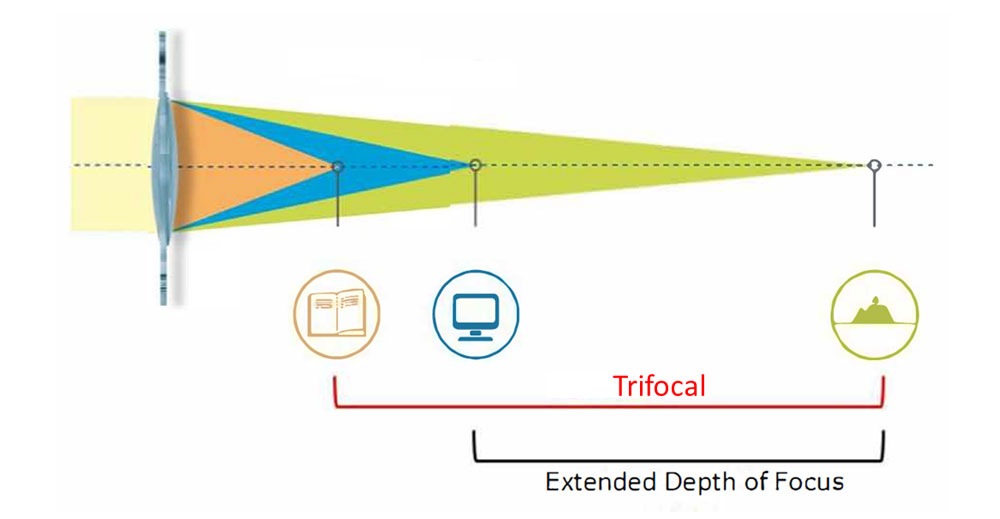
Multifocal intraocular lenses have more than one focal length to reduce dependence on glasses. Trifocal intraocular lenses aim to offer clear unaided vision for reading, computer and distance vision. Extended depth of focus lenses aim to offer clear distance and computer vision but glasses are still required for reading tasks. Multifocal lenses have to split the light between different focal lengths and so although there is less dependence on glasses, there is lower quality of vision with more haloes and glare. These symptoms are most prominent with trifocal intraocular lenses but also occur to a lesser degree with extended depth of focus intraocular lenses. These unwanted visual phenomena can be particularly troubling when driving at night. Trifocal lenses are not recommended in patients with macular disease.
Toric intraocular lenses are designed to reduce the amount of astigmatism in the visual system. Astigmatism decreases the quality of vision. Patients with significant astigmatism are offered toric intraocular lenses. These toric intraocular lenses are precisely aligned during cataract surgery to reduce the amount of astigmatism. Either monofocal or multifocal lenses can be designed to have a toric component to reduce astigmatism.

Managing cataract in patients with macula disease
There are specific considerations in managing cataract in patients with pre-existing macula disease such as age-related macular degeneration or diabetic retinopathy. With his extensive surgical experience and involvement in auditing outcomes of large numbers of patients with macula disease undergoing cataract surgery via the Fight Retinal Blindness! registry, Dr Mehta has published National evidence-based guidelines on the management of cataract in patients with macula disease.
YAG laser capsulotomy
Posterior capsular opacification describes the process by which the natural lens bag, from where the old cataract was removed and in which the new intraocular lens was placed, gradually becomes cloudy. It can occur in up to half of all patients within 5 years of cataract surgery. The symptoms of glare or blurred vision can be similar to those of cataract. YAG laser capsulotomy can be performed in the outpatient clinic to clear the clouding of the natural lens bag. This can restore vision within hours. Once treated, the posterior capsular opacification does not return.
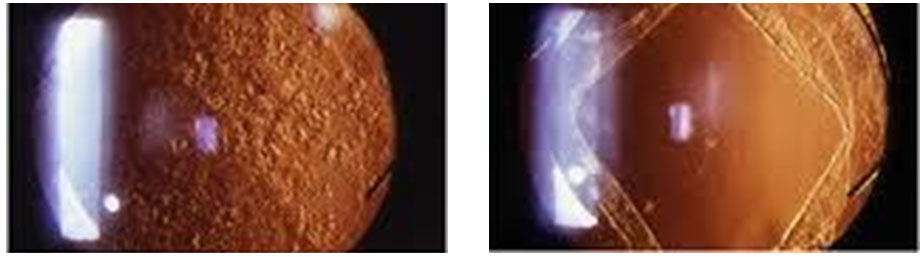
Left - Posterior capsular opacification; Right - After YAG laser capsulotomy
Any surgical or invasive procedure carries risks. The information provided here is for general educational purposes only. For more information on cataract surgery in your situation, please contact Dr Mehta's rooms.
Adjunct Professor Hemal Mehta
MBBS MD(Cantab.) FRCOphth FRANZCO
Strathfield Retina
STRATHFIELD
Eastern Suburbs Eye Specialists
BONDI JUNCTION
Norwest Eye Clinic
BELLA VISTA
Sydney Retina
MACQUARIE STREET